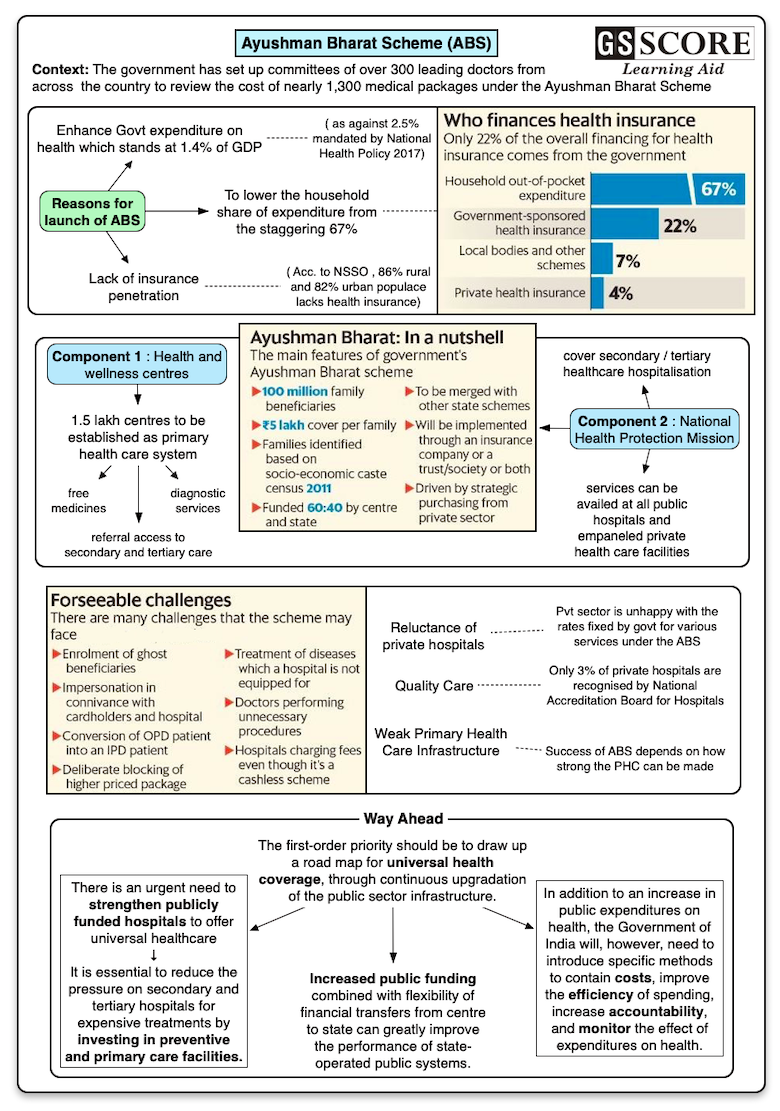
- The government has set up committees of over 300 leading doctors from across the country to review the cost of nearly 1,300 medical packages under the Ayushman Bharat Scheme.
- The committees would recommend which packages can be revised downward or upward. There are some packages which are priced on the lower side; some are on the higher side.
Issue
Context:
- The government has set up committees of over 300 leading doctors from across the country to review the cost of nearly 1,300 medical packages under the Ayushman Bharat Scheme.
- The committees would recommend which packages can be revised downward or upward. There are some packages which are priced on the lower side; some are on the higher side.
Background:
- India’s health system is already one of the most privatised in the world, with three quarters of out-patient treatment and two thirds of in-patient treatment being provided by the private sector.
- More than 17% of Indian population spend at least 10% of household budgets for health services. Catastrophic healthcare related expenditure pushes families into debt; with more than 24% households in rural India and 18% population in urban area have met their healthcare expenses through some sort of borrowings.
- India ranks as low as 145th among 195 countries in healthcare quality and accessibility, behind even Bangladesh and Sri Lanka. The country spends an abysmal 1.3 per cent of its GDP on health, way less than the global average of 6 per cent.
- Over 70 per cent of the total healthcare expenditure is accounted for by the private sector. Given the country’s crumbling public healthcare infrastructure, most patients are forced to go to private clinics and hospitals. Health care bills are the single biggest cause of debt in India, with 39 million people being pushed to poverty every year.
Ayushman Bharat
-
- This scheme is assumed to be giant leap towards providing accessible and affordable health care to the common man.
- Ayushman Bharat has labelled as the largest health scheme in the world, benefiting over 10 lakh patients since its launch, and created an atmosphere of positivity.
- With PMJAY, the government is taking healthcare protection to a new aspirational level. This would be the world’s largest government funded healthcare program targeting more than 50 crore beneficiaries.
- PMJAY primarily targets the poor, deprived rural families and identified occupational category of urban workers’ families as per the latest Socio-Economic Caste Census (SECC) data for both rural and urban areas.
- PMJAY will be an entitlement based scheme where it will be decided on the basis of deprivation criteria in the SECC database.
Analysis
- Ayushman Bharat is an integrated approach covering primary, secondary and tertiary healthcare through
- Access to Health and Wellness centers(HWCs) at the primary healthcare level.
- These centres are supposed to provide Comprehensive Primary Health Care (CPHC).
- HWCs will cover both maternal and child health services and non-communicable diseases, including free essential drugs and diagnostic services.
- Financial protection for accessing curative care at the secondary and tertiary levels through PMJAY.
Significance of Ayushman Bharat:
- HWCs can help unleash a people’s movement for a healthy India. It would be a right step in realising the goals of National Health Policy 2017.
- PMJAY will help reduce catastrophic expenditure for hospitalizations, which is mostly out of the pocket expenditure.
- Entitled families will be able to use the quality health services they need without facing financial hardships.
- It is a visionary step towards advancing the agenda of Universal Health Coverage (UHC).
- The scheme encourages hospitals to maintain certain minimum standards.
- It will enhance organisational capacity at the district and state levels, to oversee the programme.
- For insurers and third-party administrators, this is a large new market that will open up.
- The cover includes many items typically excluded in standard medi-claim: pre-existing diseases, mental health conditions, food and internal congenital diseases, among others.
- Ayushman Bharat will spur increased investment in health and generate lakhs of jobs, especially for women, and will be a driver of development and growth.
Challenges:
PM-JAY focuses on secondary and tertiary care, taking away the attention from primary care and public health-related investments. In a supply-deficit environment, raising demand will not help. The current package prices are too low to encourage private-sector hospitals to fully participate in the scheme. Hospital insurance addresses only a small amount of out-of-pocket expenditures. Finally, there is scepticism that either the required budget will not be available or provided at the expense of other critical needs etc.
Financial:
Implementation of such scale and benefit is bound to face obstacles, the most substantial of which is for it to be economically sustainable.
-
- The proposed package rates under NHPS for various treatments according to hospitals are loss-making.
- Not all the states and Union Territories are in position to raise their own share, and few have not even joined the scheme.
- The challenge of funding, therefore, remains. And without adequate budgetary commitments, the implications of pooling the financial risk for such a large segment of the population through insurers or state-run trusts or societies make the outcomes uncertain.
Human Resource:
-
- The limited and uneven distribution of human resources at various levels of health services, with up to 40 per cent of health worker posts lying vacant in some states poses a challenge to such an ambitious scheme.
- Most primary health care centres suffer from perennial shortage of doctors and even district hospitals are without specialists.
Negligence of primary healthcare:
-
- With greater emphasis on secondary and tertiary healthcare, the scheme may result in overlook of primary healthcare which is fundamental for sustainable quality healthcare.
- The scheme was nothing but an old wine in a new bottle. Ayushman Bharat does not provide out-patient department care support, which is a major component of health expenditures and is as expensive as the in-patient care.
- Besides, the policy of providing fiscal incentives to the private sector to establish hospitals in deficit areas without insulating government-owned facilities or the small and marginal hospitals that together provide 95% of hospital care will tighten the grip of corporates on secondary and tertiary markets. This will result in cost escalations — more so because of the rapid consolidation and aggregation of tertiary hospitals by foreign financial conglomerates and private equity funding agencies, impacting prices, access to tertiary care and the very sustainability of the NHPS.
Technical and Administrative:
-
- A large-scale Information Technology network for cashless treatment should be set up and validated.
- Since a majority of the families will be rural, and the secondary and tertiary public hospital infrastructure suffers from severe efficiency and accountability problems, State governments should upgrade the administrative systems.
- West Bengal, Telangana, Delhi and Odisha not joined Ayushman Bharat, the question arises whether the scheme is hurting the idea of cooperative federalism. The Seventh Schedule of the Constitution makes States responsible for hospital services. The States have their own schemes to provide financial risk protection to those seeking medical relief.
Way Forward
- There is an urgent need to strengthen publicly funded hospitals to offer universal healthcare.
- It is essential to reduce the pressure on secondary and tertiary hospitals for expensive treatments by investing in preventive and primary care facilities. Here, the 150,000 health and wellness centres of the National Health Protection Mission can play a valuable role.
- The first-order priority should be to draw up a road map for universal health coverage, through continuous upgradation of the public sector infrastructure.
- Increased public funding combined with flexibility of financial transfers from centre to state can greatly improve the performance of state-operated public systems.
- Increased public spending can also contribute to quality assurance in the public and private sectors through effective regulation and oversight.
- In addition to an increase in public expenditures on health, the Government of India will, however, need to introduce specific methods to contain costs, improve the efficiency of spending, increase accountability, and monitor the effect of expenditures on health.
|
Features of the Ayushman Bharat Scheme
|
Learning Aid
Practice Question:
Ayushman Bharat is assumed to be a giant leap towards providing accessible and affordable health care to the common man. Examine.