

- According to the fourth WHO report on Neglected Tropical Diseases (NTD), India has achieved the target for the elimination of visceral leishmaniasis (kala azar) in 82% sub-districts.
- The government has set a target of eliminating visceral leishmaniasis and lymphatic filariasis in endemic pockets by 2017.
Issue
Context:
- According to the fourth WHO report on Neglected Tropical Diseases (NTD), India has achieved the target for the elimination of visceral leishmaniasis (kala azar) in 82% sub-districts.
- The government has set a target of eliminating visceral leishmaniasis and lymphatic filariasis in endemic pockets by 2017.
- India eliminated yaws, a chronic skin disease that mostly affects poor children, in 2015. WHO recognised India as the first member state to “achieve this important milestone”.
About:
What is NTD?
- Neglected diseases are a group of parasitic and other infectious diseases that have usually been on low priority for the pharmaceutical sector and primarily affect the poorest of the poor section of community.
- The neglected diseases such as leishmaniasis, chagas disease, human African trypanosomiasis, malaria, tuberculosis and autoimmune deficiency syndrome wreak havoc on the populations of the developing world. But significantly less attention has been paid on research and development of new drugs for these neglected diseases.

Current status:
Global:
- Though the global spending on health research has increased dramatically from $30 billion in 1986 to $106 billion today, yet 90% of this allocation is being spent on the health problems of less than 10% of the world's population.
- This gap has led to the lack of drug development and innovative treatments for the diseases afflicting the poor.
- The economic burden of infectious diseases per person measured in disability- adjusted life years (DALYs) is twice as compared to that in the established market economies or the developed countries.
- Over 40% of the healthy years lost in the developing countries are attributable to communicable, maternal, and perinatal diseases, many of which never existed or have been all but eradicated in the established market economies.
- Of the total number of new drugs developed during 1975 to 2004 only 1.3% (20 new drugs) were for tropical disease and tuberculosis, which accounts for approximately 12% of diseases burden.
- WHO recommends that countries donate .01% of their gross domestic product (GDP) to research the health needs of developing countries.
- In 2017, despite increases, not a single country met this target.
- Only the US and the UK came somewhat close, underscoring that there is still a long way to go.
|
NEGLECTED DISEASES: FACTS AT A GLANCE
|
India:
- With 58 percent of leprosy cases, 40 percent of lymphatic filariasis and 34 percent of all dengue cases, India shoulders a high burden of several NTDs.
- India has also progressed well in treating lymphatic filariasis (elephantiasis), and has stopped mass drug administration in 72 endemic districts after passing evaluations.
- While some of these diseases may be unfamiliar, leprosy, kala-azar and filariasis are better known in India and are being targeted for elimination in the near future.
- India is home to a fourth of the 220.6 million children worldwide who need preventive doses of the de-worming medicines Albendazole or Mebendazole to stop worm infection.
- India has successfully eliminated certain infectious diseases—such as guinea worm, trachoma, and yaws—in recent years.
- Neglected diseases such as leishmaniasis, filariasis, leprosy, snakebite, and soil transmitted helminthic infections still pose a challenge.
Some major Neglected Tropical Diseases:
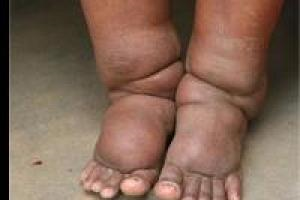
Lymphatic Filariasis
- Lymphatic filariasis (LF), commonly known as elephantiasis is a mosquito-borne parasitic disease caused by thread-like worms of the genus Wuchereriaand Brugia.
- Long-term infection progressively results in profound disfigurement and pain in the limbs and genitals as the parasites lodge in the lymphatic system causing severe swelling, secondary bacterial infections, and fever.
- Though the disease is usually irreversible, there is now evidence that treatment can alleviate symptoms of patients suffering from the disease.
- The primary goal is to stop the spread of infection by reducing worm larvae in the blood of infected persons so that mosquitoes cannot transmit the worms from one human to another.
- Mectizan and albendazole is part of the strategy as the combination kills off the microfilariae.
- WHO recommends a single, annual dose over five years of Mectizan and albendazole in onchocerciasis-endemic countries in Africaand in Yemen, or Mectizan and diethylcarbamazine in all other LF-endemic countries to interrupt transmission.
Trachoma
- Trachoma is the world’s leading infectious cause of blindness.
- It is caused by infection from the bacterium chlamydia trachomatis which spreads through contact with eye discharge from an infected person – via hands, towels, sheets and, in some cases, eye-seeking flies, and thrives where there is poor sanitation and limited access to water for personal hygiene.
- Approximately 200 million people worldwide living in trachoma-endemic districts and 3.2 million people need surgery to avoid blindness because of trachoma.
Leprosy
- Leprosy is a chronic infectious disease caused by Mycobacterium leprae.
- The disease mainly affects the skin, the peripheral nerves, mucosa of the upper respiratory tract and also the eyes.
- Leprosy is curable and treatment provided in the early stages averts disability.
- Multidrug therapy (MDT) treatment has been made available by WHO free of charge to all patients worldwide since 1995, and provides a simple yet highly effective cure for all types of leprosy.
Leprosy Facts
- Official figures show that 214 783 new cases of leprosy were reported during 2016. Globally, the number of new cases detected annually has remained stable, at around 220,000, in recent years.
- leprae multiplies very slowly and the incubation period of the disease is about five years. Symptoms can take as long as 20 years to appear.
- Leprosy is not highly infectious. It is transmitted via droplets, from the nose and mouth, during close and frequent contacts with untreated cases.
- Untreated, leprosy can cause progressive and permanent damage to the skin, nerves, limbs and eyes.

LEISHMANIASIS or KALA-AZAR
- Leishmaniasis is endemic in 88 countries with an estimated 350 million people at risk.
- Around 2 million people become ill with leishmaniasis every year. Only 30% of this number is officially reported.
- The most severe form, visceral leishmaniasis or kala-azar, is a fatal disease.90 % cases occur in five developing countries: India, Bangladesh, Brazil, Nepal and Sudan.
- Kala-azar also occurs in Europe. In Southern Europe, over 1,600 people have been diagnosed as infected with both kala-azar and HIV up to early 1999.
AIDS
- AIDS is caused by the human immunodeficiency virus (HIV).
- AIDS can be treated with antiretroviral drugs that stop the virus from replicating, but do not kill it. This treatment is still not widely available in developing countries.
Analysis
India’s success in fighting NTDs:
- According to the G-Finder Report (most comprehensive analysis of ND released by Policy Cures Research) India scaled its contribution by 38% to $76 million in 2017, upholding its position as the fourth-largest public funder globally.
- A large part of this increase came from ICMR (Indian Council of Medical Research), which substantially increased its investments in malaria, TB and other neglected tropical diseases.
- For the first time ever, ICMR has been placed in the top four largest funders of TB research and development (R&D).
- It is also the only organization from low- and middle-income countries to feature in the top 12 funders.
- The Biotechnology Industry Research Assistance Council has developed an ecosystem of programmes and schemes that provide holistic support to startups and small and medium enterprises.
- The new triple drug therapy for eliminating lymphatic filariasis (LF) was launched in December 2018.
- Unlike traditional LF treatments, a single dose of the new triple-drug therapy is enough to kill the adult worm, making it significantly faster, easier and cheaper to cure people.
- India, which bears 40% of the global disease burden, is the first country in South-East Asia to introduce the new treatment regimen.
- Two Indian vaccines for typhoid and rotavirus have received WHO prequalification.
- India has also made strides developing affordable and accurate diagnostic tools, including a point-of-care molecular detection platform that can detect a variety of infectious agents.
Recent policies in health sector and their drawbacks:
- The National Policy on Treatment of Rare Diseases (2018) includes infectious tropical diseases and identifies a need to support research on treatments for rare diseases. It has not yet prioritised diseases and areas for research funding or how innovation would be supported.
- The National Health Policy (2017) sets an ambition to stimulate innovation to meet health needs and ensure that new drugs are affordable for those who need them most, but it does not specifically tackle neglected diseases
- The Draft National Pharmaceutical Policy (2017) states that one of its objectives is to create an enabling environment to develop and produce innovator drugs, but the policy does not mention drugs for neglected tropical diseases.
- The National Biotechnology Development Plan (2015-2020) seeks to encourage the preclinical and clinical development of vaccines against rotavirus, cholera, typhoid, rabies (human (DNA) based), malaria, dengue, tuberculosis, and Japanese encephalitis.
- The National Intellectual Property Rights Policy (2016) states that it will encourage publicly funded R&D institutes and industry to develop affordable drugs for neglected diseases but does not spell out how it will do so. There has been no activity reported in this area.
- The Open Source Drug Discovery programme was set up by the Council of Scientific and Industrial Research for new inventions for the prevention, diagnosis, and treatment of common diseases in India. This programme is no longer being funded. It could have served as a platform to discover new drug targets and drugs for infectious and non-communicable diseases.
- The Science, Technology, and Innovation Policy (2013) does not mention research on neglected diseases.
Way forward
- It is time for India to establish a comprehensive policy on neglected diseases that paves the way for greater funding and mechanisms to support research and innovation.
- Creating an enabling environment for research and innovation will be crucial if India is to achieve the target set in sustainable development goal 3.3 to end epidemics of neglected tropical diseases by 2030.
- WHO in June 2017 adopted snakebite envenoming as a 'category A' neglected tropical disease (NTD).
- A disease is considered ‘eliminated’ when the prevalence rate is less than 1 case per 10,000 population size.
Learning Aid
Practice Question:
- A comprehensive policy for neglected diseases research in India is needed to foster innovation in drugs, diagnostics, and vaccines, critical for evolving needs of elimination programmes. Discuss
- What are Neglected Tropical Diseases (NTDs)? How they affect India illustrate with examples. Also suggest what measures should India take to eliminate NTDs?


