In its recently released World Malaria Report 2018, the World Health Organisation (WHO) has reported a sharp decline in the number of malaria cases in India.
Issue
Context
- In its recently released World Malaria Report 2018, the World Health Organisation (WHO) has reported a sharp decline in the number of malaria cases in India.
- India has been found to be the only country to report such decline, registering a 24 percent decrease in 2017 as compared to 2016.
About
Key highlights
- India and 15 other countries in sub-Saharan Africa accounted for almost 80 per cent of the malaria cases reported globally last year.
- Five countries account for nearly half of all malaria cases worldwide i.e. Nigeria (25 per cent), Democratic Republic of the Congo (11 per cent), Mozambique (5 per cent), India and Uganda (4 per cent) both.
- India accounted for 52 per cent of deaths that occurred outside the WHO African Region and all this happened despite ‘impressive gains’.
- By leading the world in malaria case reductions in 2017, India is now no longer among the top three countries with the highest malaria burdens.
- However, the report also noted that a whopping 1.25 billion Indians remain at risk of contracting the mosquito-borne disease. India has set a target of being malaria-free by 2027 and eliminating the disease by 2030.
Background
Malaria
- It is a life-threatening disease caused by parasites belonging to the Plasmodium genus, which are transmitted to people through the bites of infected female Anopheles mosquitoes. The mosquito-borne blood disease is preventable and curable.
- Plasmodium parasite infects a variety of species and different types of Plasmodium genus replicate at different rates, changing how quickly the symptoms escalate, and the severity of the disease.
Five types of Plasmodium parasite can infect humans. These occur in different parts of the world. Some cause a more severe type of malaria than others. Once an infected mosquito bites a human, the parasites multiply in the host's liver before infecting and destroying red blood cells.
|
Analysis
India’s Strategy to Eliminate Malaria
- Malaria is a major public health problem in India. Malaria interventions are highly cost-effective and demonstrate one of the highest returns on investment in public health.
- In countries where the disease is endemic, efforts to control and eliminate malaria are increasingly viewed as high-impact strategic investments that generate significant returns for public health, help to alleviate poverty, improve equity and contribute to overall development.
- From the beginning of the 21st century, India has demonstrated significant achievements in malaria control with a progressive decline in total cases and deaths.
National Framework for Malaria Elimination 2016-2030
Aim:
In line with the WHO Global Technical Strategy for Malaria 2016–2030 (GTS) and the Asia Pacific Leaders Malaria Alliance Malaria Elimination Roadmap, it aims to:
- Eliminate malaria (zero indigenous cases) throughout the entire country by 2030; and
- Maintain malaria-free status in areas where malaria transmission has been interrupted and prevent re-introduction of malaria.
Objectives:
- Eliminate malaria from all 26 States including 15 low (Category 1) and 11 moderate (Category 2) transmission States/Union Territories (UTs) by 2022;
- Reduce the incidence of malaria to less than 1 case per 1000 population per year in all States and UTs and their districts by 2024;
- Interrupt indigenous transmission of malaria throughout the entire country, including all 10 high transmission States and Union Territories (Category 3) by 2027; and
- Prevent the re-establishment of local transmission of malaria in areas where it has been eliminated and maintain national malaria-free status by 2030 and beyond.
Short term milestones
- By end of 2016, all states/UTs are expected to include malaria elimination in their broader health policies and planning framework
- By end of 2017, all states are expected to bring down API to less than 1 per thousand population
- By end of 2020, 15 states/UTs under category 1 (elimination phase) are expected to interrupt transmission of malaria and achieve zero indigenous cases and deaths due to malaria.
- District as the unit of planning and implementation
- Focus on high endemic areas
- It is also envisaged that in states with relatively good capacity and health infrastructure, such as, Gujarat, Karnataka and Maharashtra, accelerated efforts may usher malaria elimination sooner - within two to three years.
Challenges in Malaria control
- Population movements, often uncontrolled across states/UTs, and sharing of large international borders with neighbouring malaria endemic countries: There are 36 states and union territories in India, most of which share large borders with each other. This often leads to the spread of malaria from one state to another due to movement of populations. With different administrative structures and variable functioning of health systems in each state, management of malaria in such mobile and migrant populations becomes difficult.
- Additionally, some of the high-endemic states including north-eastern states share their border with neighbouring countries such as Myanmar and Bangladesh where malaria is still prevalent and there is a persistent threat of influx of malaria cases from these countries.
- There is also a growing threat of the spread of malaria multi-drug resistance including ACT resistance as a result of sharing these international borders.
- Shortage of skilled human resources: The programme is adversely affected by an insufficient number of sanctioned posts of health workers and other programme staff in different parts of the country. For instance, there are about 40,000 multipurpose health workers (MPWs) against approximately 80,000 sanctioned posts for nearly 150,000 sub-centres across the country.
- Insecticide resistance: The extensive use of insecticides, particularly DDT, under the vector control programme controlled malaria to a great extent but exerted high selection pressure on the vector population to develop resistance.
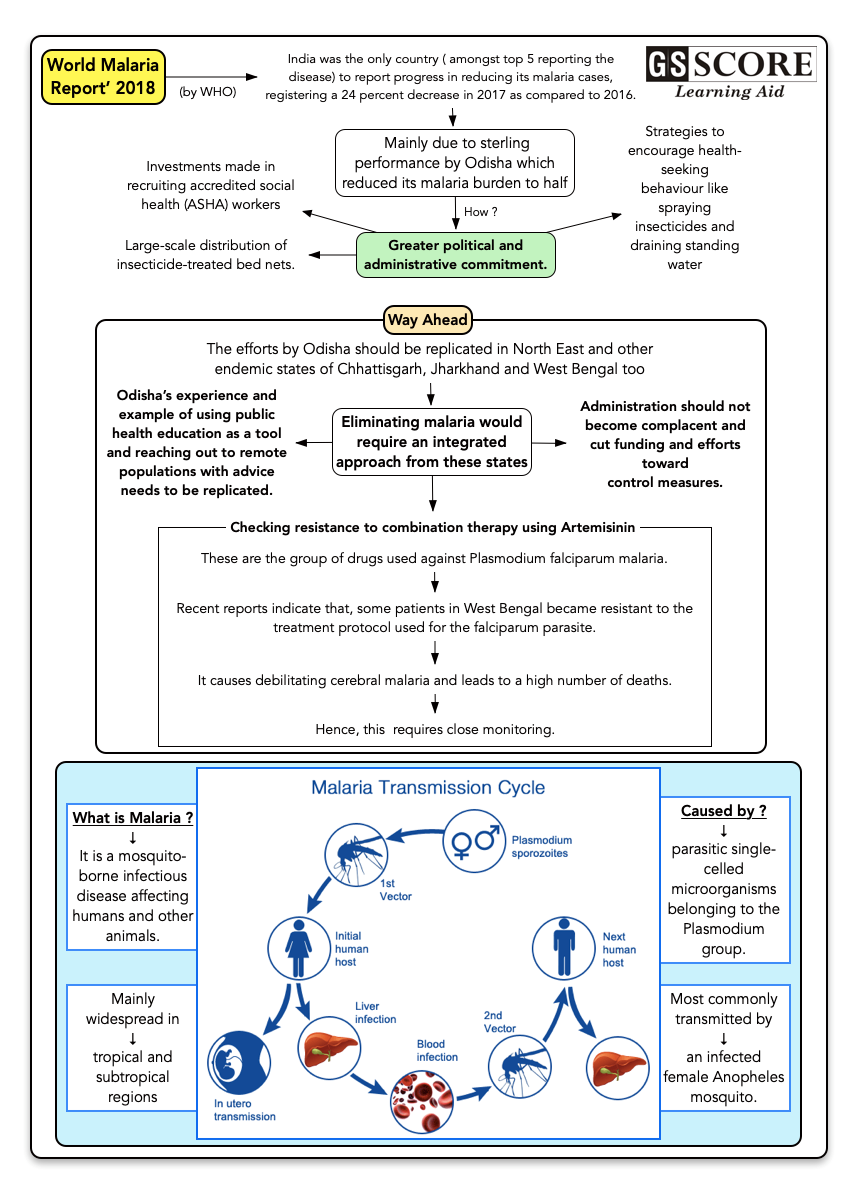
Odisha success story: The WHO report stated that India registered a 24 per cent reduction in cases largely due to substantial declines of the disease in the highly malarious state of Odisha, home to approximately 40 per cent of all malaria cases in the country.
Way Forward
- Eliminating malaria requires an integrated approach, and this should involve Chhattisgarh, Jharkhand and West Bengal, which have a higher burden of the disease.
- Odisha’s experience with using public health education as a tool and reaching out to remote populations with advice needs to be replicated elsewhere.
- Given that emerging resistance to treatment has been reported in Myanmar, among other countries in this belt, there is a need for a coordinated approach to rid southern Asia of malaria.
- To eliminate malaria from India by 2030 will require additional resources. At present, public spending on malaria control in India represents a small proportion of the country’s overall expenditure on health.
- There may be scope to increase the funding to a level that will reduce significantly the burden currently being placed on households by their out-of-pocket payments for the diagnosis and treatment of malaria.
Learning Aid
Practice Question:
As per World Malaria Report 2018, India has witnessed a sharp decline in the number of malaria cases. In this context, critically discuss India’s strategy to eliminate malaria by 2030.